EDITORIAL
A special issue of the Sechenov Medical Journal (No. 2 for 2020) dedicated to COVID-19, attracted great interest within the professional community with a wide range of readers, and opened up the opportunity for a productive discussion of the results obtained by leading Russian experts.
ОBSTETRICS AND GYNECOLOGY
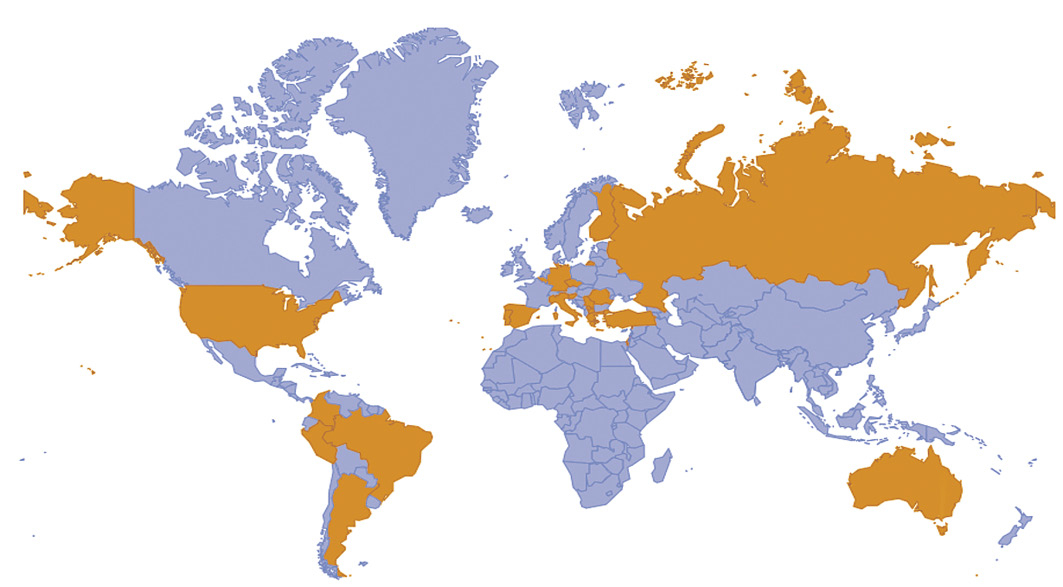
The World Association of Perinatal Medicine (WAPM) study on the COrona VIrus Disease 2019 (COVID-19) was an international, retrospective cohort study that included pregnant women tested positive with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection between February and April 2020. The study involved 73 centers from 22 countries. The WAPM study included 388 singletons, viable pregnancies, positive to SARS-CoV-2 at real-time reverse-transcriptase-polymerase-chain-reaction nasal and pharyngeal swab. The majority of the included women were symptomatic. The occurrence of maternal adverse events was significantly higher in symptomatic, compared with asymptomatic pregnant women. Women carrying high-risk pregnancies (either preexisting chronic medical conditions in pregnancy or obstetrical disorders occurring in pregnancy) were at a higher risk of hospital admission, presence of severe respiratory symptoms, admission to the intensive care unit, and invasive mechanical ventilation. As per maternal outcomes, the occurrence of fetal and neonatal adverse events was significantly higher in symptomatic, compared with asymptomatic pregnant women. The incidence of a composite adverse fetal outcome was significantly higher when the infection occurred in the first trimester, and in fetuses with lower birthweight.
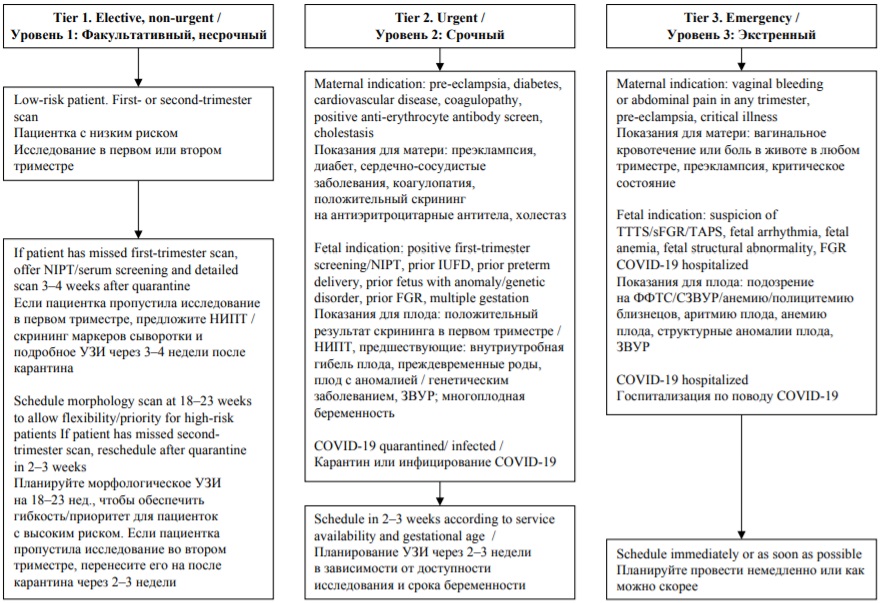
The coronavirus disease 2019 (COVID-19) pandemic has posed unprecedented challenges for the delivery of high-quality obstetric services to both SARS-CoV-2 positive and negative women. The initial epidemiological pressure, especially in the most affected areas of China and Italy, led the local health services to defining care pathways based on the organizational and logistical availability of the moment. Currently, some aspects of clinical care practices and the management of women with suspected or confirmed SARS-CoV-2 virus infection are well established. The aim of this review article is to provide an outline of the suggested organization of obstetric units during the COVID-19 pandemic, and to mention the challenges we had to face at our institution.
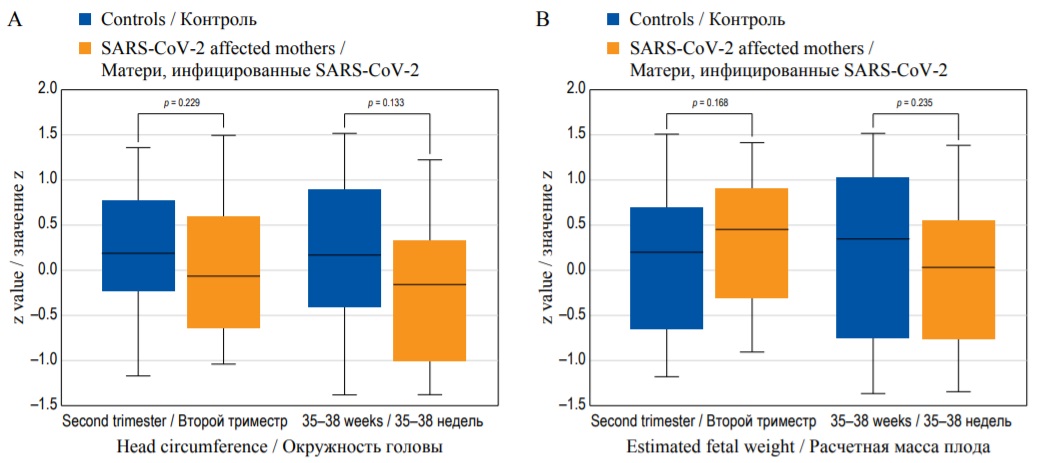
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is a virus that, having crossed species, has caused human disease from 2019 - COrona Virus Disease 2019 (COVID-19). Pregnant women are potentially at high risk of contracting SARS-CoV-2 infection when compared to non-pregnant matched controls. Pregnancy is also complicated with a higher risk of developing severe SARS-CoV-2, including respiratory diseases, admission to the intensive care unit and mortality, even after adjusting for confounding risk factors. Moreover, data on the effect on fetal outcome including preterm delivery and perinatal morbidity are still conflicting, the risk of vertical transmission (i.e., transmission of SARS-CoV-2 from the mother to the fetus or the newborn) is considered low but there is evidence that a significant proportion of placentas where SARS-CoV-2 occurred during pregnancy show histopathological findings suggesting placental hypoperfusion and inflammation. In this review we will present the available data on the effects of SARS-CoV-2 infection on fetal growth and maternal hemodynamics
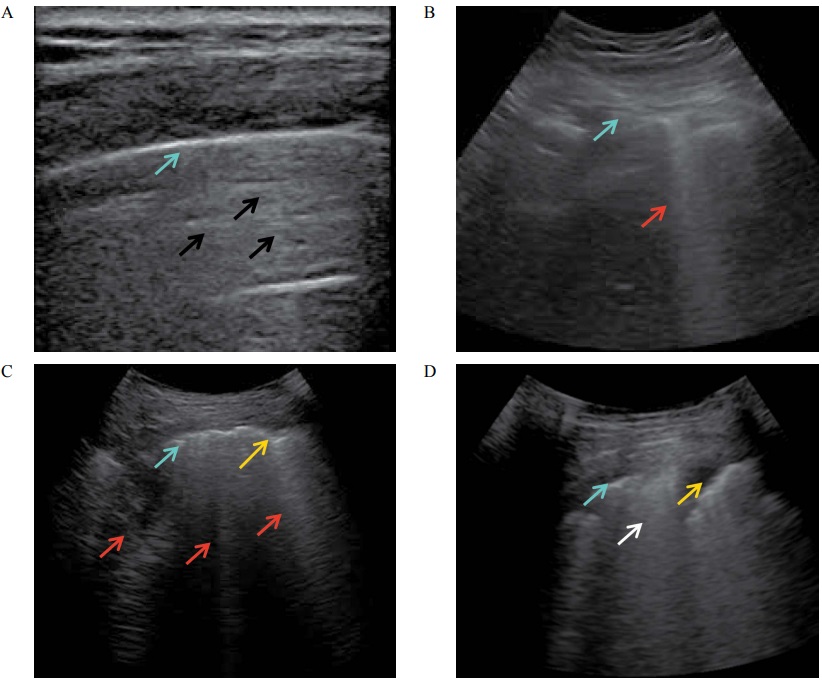
Lung ultrasound has been recognized as a valid imaging method for diagnosing and monitoring COVID-19 pneumonia in pregnant women. The present review aimed to summarize the main findings reported in the literature and international guidelines on the role of lung ultrasound in the care of pregnant women affected by COVID-19. A search strategy was developed and applied to PubMed, Scopus, Web of Science and EMBASE to identify previous papers reporting the utility of ultrasound in diagnosing and monitoring COVID-19 pneumonia. The search retrieved 369 articles and 23 of these were selected for analysis. The articles mainly focused on the definition of the procedure, development of training programs for obstetricians managing pregnant women with suspicion of COVID-19 and definition of scoring systems. The clinical applications of lung ultrasound in this setting have also been described. This review could encourage obstetricians to learn lung ultrasound to use during critical events like a pandemic.
The coronavirus SARS-CoV-2 (COVID-19) infection is a public health emergency of international concern. Pandemics pose a challenge to psychological resilience and can have an adverse impact on mental health. The impact of the ensuing social isolation and loneliness imposed by quarantine along with the worries about the risks of the infection and its economic fallout would appear likely to affect the mental health of the population. It has been reported that women are more likely to experience anxiety and depression symptoms during COVID-19 than men. COVID-19 pandemic had a profound impact on the level of anxiety and depression of pregnant women according to their basal level and pregnancy characteristics. Antenatal mental disorders may be a risk factor for maternal mental health problems such as an increased likelihood of postnatal depression and adverse obstetric and developmental outcomes. Effective coping strategies are associated with better psychological wellbeing during the COVID-19 pandemic, including reduced anxiety and depression. The increased risk of mental disorders due to COVID-19 requires policies to be developed to address prenatal and postpartum care to promote maternal-child wellbeing outcomes.
The physiological and anatomical clinical characteristics of pregnant women make them susceptible to complications caused by coronavirus disease (COVID-19). Increased coagulation and risk of thromboembolic phenomena are common during pregnancy; they are further enhanced when associated with a thrombogenic pathology such as in COVID-19. The treatment of COVID-19 is controversial and limited, even for non-pregnant patients. During pregnancy, the options are even more restricted due to the teratogenicity of some drugs and anatomical and physiological difficulties, especially in advanced pregnancy in patients with respiratory failure. Therefore, the focus of treatment for pregnant patients should be centered on isolation, monitoring fetal and maternal vital signs, uterine activity, and general maternal-fetal well-being. The prescription of drugs and management orientation should be based on gestational age and maternal clinical conditions. The optimal type of delivery is guided by obstetric indications and COVID-19 disease severity. Breastfeeding should be encouraged with the use of masks and hand hygiene. The treatment of pregnant women with COVID-19 brings important peculiarities that should be considered in order to make better decisions for preserving the health of the mother and fetus.
There has been changing guidance from national and international professional associations, national and international non-governmental organizations, and health officials in national governments for obstetrician-gynecologists about COVID-19 vaccination of pregnant women and women who are planning to become pregnant. in this paper, we provide an ethical framework that provides the needed guidance to decision making about recommending COVID-19 vaccination to these patients. the unique feature of this ethical framework is that it is based on professional ethics in obstetrics and gynecology. We begin with an account of three key components of professional ethics in obstetrics and gynecology and how they are pertinent to the ethics of making recommendations that should be understood in obstetric and gynecologic practice generally. We then identify the implications of this overview for the specific topic of the ethics of recommending COVID-19 vaccination.
ISSN 2658-3348 (Online)